Postural Orthostatic Tachycardia Syndrome, called “P.O.T.S.,” is a relatively new and growing diagnostic label. Let’s take a look at this diagnosis and how to stop P.O.T.S.
What is P.O.T.S.?
Individuals with P.O.T.S. experience a rapid increase in their heart rate when they stand up, often accompanied by low blood pressure symptoms. These symptoms include heart palpitations, altered balance, fatigue, general anxiety, headaches, neck tightness, impaired concentration or memory, lightheadedness or dizziness, and syncope (passing out).
They may also suffer from non-orthostatic symptoms such as chest pain or tightness, air hunger, constipation, heartburn, IBS, insomnia, painful menstrual cramps, and premenstrual syndrome.
The rapid increase in the heart rate after standing is the unique characteristic of this condition, and it predominantly occurs in young women of reproductive age. Still, it can also occur in young males.
How Does P.O.T.S. Develop?
People are not born with P.O.T.S. It often develops following an injury to the brain or autonomic nervous system.
Most people who experience an injury to their autonomic nervous system will experience symptoms from low blood pressure symptoms to their brain. This is referred to as orthostatic intolerance. Persons diagnosed with P.O.T.S. have two particular injuries. The first is orthostatic intolerance, and the second is damage to the normal compensatory heart rate increase when standing. When someone with an intact autonomic nervous system stands, their heart rate will often increase by ten beats per minute to compensate for the downward pressure of gravity.
When someone with only orthostatic intolerance stands up, their heart rate may go up 20-30 beats per minute. The increase in heart rate is a compensatory mechanism by the nervous system to maintain proper blood pressure within the brain. But when someone with P.O.T.S. stands up, the normal heart rate compensatory increase mechanism is damaged, so the heart rate skyrockets with increases of 40-80 beats per minute.
The rapid heart rate symptoms typically occur quickly when the person stands up or stands still. The injury causing the blood pressure regulation and compensatory heart rate increase often results from physical or emotional traumas, or surges in inflammatory stress from COVID, surgical stress, vaccinations, pregnancy, or fractures of large bones.
How is P.O.T.S. Diagnosed?
The current diagnostic criteria for P.O.T.S. is a heart rate increase of 30 beats per minute (bpm) or more, or over 120 bpm, within the first ten minutes of standing, without a significant drop in measured blood pressure. Standing for ten minutes is a very simple test for P.O.T.S., but many patients are diagnosed by a cardiologist using a tilt-table test.
While an abnormal heart rate diagnostically determines P.O.T.S., it is also reasonably common for P.O.T.S. patients to notice a drop in blood pressure upon standing. But some P.O.T.S. patients have no change in their blood pressure, or they may even experience an increase in their blood pressure when they stand up. Those conflicting blood pressure readings can be confusing for people who do not understand the mechanics of what is malfunctioning with the body.
One crucial point to know is that POTS is not a discrete diagnosis. It is considered a “syndrome.” The medical use of the word “syndrome” implies a lack of a well-defined understanding of the disorder. In other words, there are probably various issues causing the disorder. What has become more evident is that P.O.T.S. is one form of autonomic nervous system dysfunction.
The second important point is that similar to all new syndromes, health professionals may tend to focus more on labels than finding practical answers to help patients feel better. Fortunately for patients suffering from P.O.T.S., improvement or recovery from their underlying autonomic damage is now possible.
The Nervous System Problem
To understand how I begin to stop P.O.T.S. (a palindrome, as P.O.T.S. spelled backward is STOP), I will go back to the beginning to teach you about the nervous system problem and the autonomic answers.
The mechanical problems involved with P.O.T.S. involve the dysfunction of the autonomic nervous system, which is the brain’s master control mechanism over the body. The autonomic nervous system coordinates and regulates all organ functions, blood pressure control, metabolism, hormone regulation, and inflammation.
Autonomic dysfunction occurs when the nerves that carry the information from the brain and spinal cord to the heart, bladder, intestines, sweat glands, blood vessels, hormonal organs, and the immune system no longer work properly. Damage or disruption to autonomic function causes those bodily things not to function correctly and leads to a wide range of symptoms.
The autonomic nervous system controls our heart and adapts our blood pressure and pulse rate to changes in our posture and physical stress. Erratic heart rhythms, excessively high or low heart rates, and abnormal blood pressure readings are connected to autonomic nervous system dysfunction.
The autonomic nervous system has two main branches. We know them by the type of brain commands they carry, such as the sympathetic (“fight or flight”) and the parasympathetic (“rest and digest”) branches. The sympathetic and parasympathetic branches feed into the heart and modulate the heart’s natural rhythm and contractility.
Our normal resting heartbeat should be 60 to 70 beats per minute; the parasympathetic branch manages that rate. The parasympathetic branch makes the heartbeat go fast or slower, while the sympathetic branch is more involved with the strength of the heart’s contractions.
Stages of Autonomic Dysfunction
There are five stages in autonomic dysfunction, and autonomic testing can reveal subtle and progressive autonomic dysfunction as the brain becomes increasingly unable to modulate the heart. Parasympathetic dysfunction results in an increase in cardiac arrhythmias, and P.O.T.S. is also related to the weakening of the sympathetic branch in particular.
As parasympathetic function weakens, the EKG portion of autonomic testing indicates whether the person has moved into atrial fibrillation (A-fib), atrial flutter, has low heart rate variability or has progressed to a point where they are now at risk of sudden cardiac death (Cardiac Autonomic Neuropathy or CAN).
The unique feature of P.O.T.S., the rapid heart rate, is from the combined effects of poor regulation of the heart rate response to the inadequate generation of blood pressure and oxygen delivery upwards into the brain when the person is upright.
-
Posture
The person suffering from the rapid heart rate symptom is having difficulty adapting their blood pressure and their pulse against the stress of gravity. The problem with the change in their posture is the letter “P” in P.O.T.S.
In other words, when someone stands up, their body should compensate for gravity by delivering a perfectly timed increase of blood pressure and blood oxygen upward to their brain. When their autonomic nervous system branches work correctly, blood pressure and oxygen delivery usually occur, and no symptoms occur.
But when the autonomic nervous system is damaged, and the sympathetic and parasympathetic branches no longer function correctly, the person may feel the rapid heart rates of P.O.T.S. and experience swings in blood pressure.
-
Orthostatic Intolerance
The letter “O” (orthostatic) in P.O.T.S. stands for orthostatic intolerance, which is the development of symptoms when they move to an upright position or after sitting or standing up for an amount of time.
-
Tachycardia
The other feature of P.O.T.S., the elevated heart rate, is a tachycardia response to the drop in the blood pressure upward to the brain. Tachycardia is the letter “T” in P.O.T.S. It is a hydraulic malfunction with one’s cerebral blood pressure regulation, making their pulse very high.
In less severe cases of autonomic dysfunction (stages 1 -3), the person may feel a head rush, get a little dizzy or lightheaded, or feel anxious when standing upright or changing their posture.
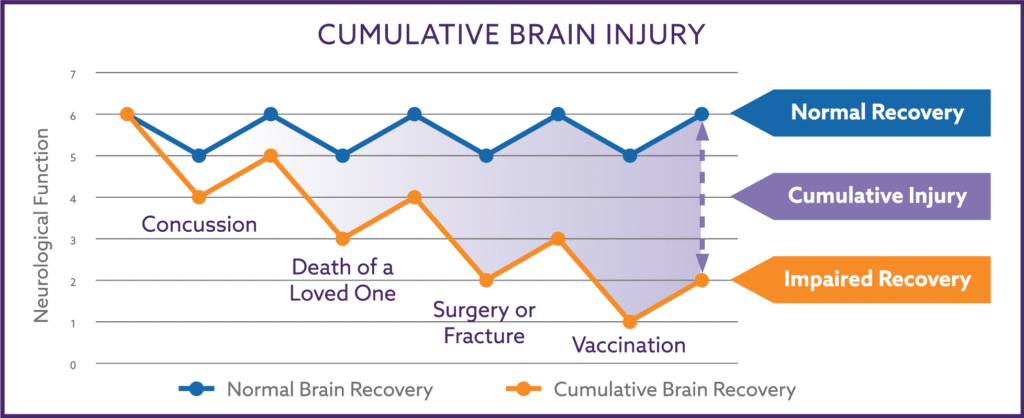
The functional damage to the autonomic nervous system that triggers P.O.T.S. symptoms may be triggered by physical trauma to the brain (falls, concussions, bumps to the head), emotional traumas that profoundly impact the individual (death of a loved one, intense fear, bullying), or from prolonged inflammatory reactions that may result after a vaccination, surgery, or even from allergy testing or shots.
How to STOP P.O.T.S.
I have discovered an approach that allows the autonomic nervous system to repair itself. Referred to as The Nemechek Protocol, my approach reduces the chronic inflammation within the body and brain, allowing the brain’s natural repair and rejuvenation mechanisms to function more appropriately. It is a natural process that allows a person to begin repairing the underlying autonomic nervous system injury. This is possible to do without long-term medications in most individuals by down-regulating metabolic (chemical) inflammation through short-term medications, a limited number of omega-3 nutrients for the brain, the elimination of omega-6 vegetable oils from the diet, by controlling bacterial overgrowths in the intestinal tract, and in some people by using vagus nerve stimulation.
A Shift in Diet
Something as simple as a shift in the diet to more omega-3 fatty acids (most easily accessible in fish oil) and a reduction of inflammation-promoting omega-6 fatty acids (vegetable oils) helps to create a healthier inflammatory environment in the body that improves the brain’s capacity to repair itself. It has been my experience that a consistent change in these dietary chemicals in someone’s daily food is absolutely mandatory for achieving or maintaining autonomic nervous system health.
Bioelectric Medicine
I have also seen the powerful effects of bioelectric medicine on the central nerve of the autonomic nervous system, which is the Vagus (or “vagal”) nerve. The vagus nerve carries information from the organs to the brain, which is instrumental in regulating inflammation in the autonomic nervous system. While we typically think if we stimulate something, we are turning something “on,” when it comes to the autonomic vagus nerve, this stimulation actually helps turns inflammation “off.” Stimulating the vagus nerve is one additional tool to calm down the inflammation that prevents the brain and nervous system from healing the underlying injury (physical and emotional trauma, inflammatory stress) responsible for the symptoms of P.O.T.S.
When inflammation lowers and cells naturally function again, the body finally heals. When the autonomic nervous system improves or repairs, the two branches work together again in balance. Then, the symptoms with the change in posture (the “P”) dissipate because the body can once again generate enough blood pressure and oxygen upward to the brain.
This improved blood pressure and oxygen delivery to the brain further resolves the orthostatic intolerance (the “O”) and the abnormal tachycardia response from the heart (the “T”). When the symptoms are gone, the syndrome (the “S”) is gone.
Autonomic Disorders
There are two other types of autonomic disorders with low brain oxygen features that a P.O.T.S. patient may or may not experience. One is Vasovagal Syncope (VVS), another autonomic disorder causing low oxygen delivery to the brain. Still, the main symptom of VVS is passing out when startled or stimulated (needle puncture from a blood draw, sight of blood, a negative visual experience). The other autonomic disorder causing low brain oxygen levels is neurogenic orthostatic hypotension. In the case of orthostatic hypotension, individuals have very low blood pressure readings in the arm and frequently feel faint or lightheaded.
There is no magic pill or quick fix for repairing the autonomic nervous system; individual results will always vary. Reversing autonomic nervous system damage requires a sustained reduction in the patient’s metabolic (chemical) inflammation for years. Maintaining recovery and healing from new autonomic injuries will require maintaining a lower, healthier inflammatory state in the body throughout their lifetime.
A Little Encouragement
If you or a family member have been diagnosed with P.O.T.S. or any of these other conditions causing low brain oxygen, the encouraging news is that these things are reversible. The key to recovery is to work to resolve the underlying sympathetic and parasympathetic dysfunction and not just mask the symptoms.
At first glance, P.O.T.S. seems like just a cardiac issue. However, it actually involves the brain, the nervous system, the intestinal tract, the production of stem cells, inflammation, and the chemicals in a person’s diet.
Therefore, the reduction of brain inflammation, the reversal of intestinal bacterial overgrowth, and the electrical stimulation of the autonomic nervous system help reverses the underlying dysfunction and eliminate symptoms.


Is the protocol book for Autism the same one you would use for a adolescent patient with POTS?
Yes
Hi Dr Nemechek,
I have severe POTS and am bedridden . I’m saving up to have a skype consult with you from the UK, but wondered while I’m waiting if there’s anything I can get started with to help me get out of bed and more upright? Perhaps if I start omega 3 fish oils and eliminate all omega 6 oils? If so how much fish oil should I take? Thank you so so so much, Josie
The protocol I developed for adults was later adapted for autism.
Reading our autism protocol book will outline the science and gives you the doses I recommend for adults. The dosing for aults with and without autism are the same.
You can purchase a copy at https://autonomicrecovery.shop
Hello Dr. Nemecheck,
My 14 year old daughter has just been diagnosed with Mast Cell Activation Syndrome and Vasovagal Syncope. I have MCAS as well. We live on the East Coast and both are unable to travel due to reactions. I started her on the oils, but she has a histamine reaction to the fish oil and the EVOO. Is there a way to have a digital visit with you without traveling across country?
I am sorry, we no longer provide Skype or phone sessions for U.S. residents.
I would like to add that the histamine reactions you are seeing are secondary to SIBO and not due to fish oil or olive oil per say.
Hello Dr Nemechek My seven year old granddaughter has been recently diagnosed with POTS using the tilt table test at the Great Ormond Street Hospital in London. She was diagnosed with Ehlers Danlos a number of years ago and has high functioning autsm. The cardiologist has prescribed a beta blocker, salt and fluids. She has not started the beta blocker yet, but we have been told that this drug will only take the edge off of the symptoms. She has a severe case of POTS and we have been warned that she could end up in a wheelchair. Since birth,… Read more »
Yes we can help.
She is crawling around the house because standing causes too much unpleasant lightheadedness when fully upright.
The propranolol might make this worse.
Start my protocol and set up a Skype visit.
I was tested positive for SIBO (methane dominant) 2 years ago and was treated with Rifaximin and Neomycin (they often substitute if with Flagyl). It is believed in Australia that only the combo of both can treat it properly. Now I am facing full-on POTS syndrome and going to follow your protocol. Would you say Rifaximin still works for methane SIBO? Thank you for your time and all the work you are doing.
The test is extremely inaccurate and I don’t use it.
What’s your opinion on the drug Fludrocortisone for someone with POTS suffering dizzy spells, fatigue, palpitations etc?
It’s helpful sometimes. Increases intravascular volume and can reduce some of the orthostasis.
Hello,
Have you ever had any of your patients with POTS have stem cell treatment? What’s your thoughts on this, are there any proven benefits?
Thanks
I do not recommend stem cell therapy because in their present form they are ineffective, costly and potentially dangerous. There is a growing chronic inflammatory condition believed to be affecting most everyone worldwide. It is often referred to as inflamm-aging or chronic metabolic inflammation, and is manifest as the chronic and highly abnormal secretion of pro-inflammatory cytokines. Humans make stem cells throughout their lives and some research suggest the rate of production even increases as we age. Unfortunately the inflammatory cytokines released from inflamm-aging prevents our natural stems cells from working. They also prevent infused stem cells from working. In… Read more »
If POTS started from a bad case of mono and I’m still testing positive years later for chronic reactivated EBV is that something you would address specifically or does following the protocol allow your body to take care of the virus itself once it’s restored function?
Chronic re-activated EBV is really a misunderstanding of the EBV tiers. Any source of inflammation can falsely make make some antibody titers look like re-activation (+ IgM).
If you were under my care, I would ignore the testing and just reverse the autonomic dysfunction.
Thanks so much for responding! That makes sense! I’m flying out to see you in December!
Find your work very interesting. My daughter has Genetic type 1 von willie brand, and they suggest no fish oil. What are your thoughts on this. She suffers with low blood pressure normally and what I would say is vasovagel syncope a few times a year. noticed syncope when it occurs is after urination. Have you heard of Emrys Goldsworthy in Australia re vagus nerve stimulation and red light therapy
You’ll have to discuss this with your specialists. My question to them would be do they tell their patients not to consume fish as well as fish oil? Are there reported causes of more bleeding from those with high fish intakes (eskimo’s for instance)
Hello D.O. I am very interested in starting your protocol. I am in the US Army, and I believe my issues may stem from injuries and inflammation and a horrible diet. I am getting out soon, and my desire is to become a Fire Fighter however I don’t want to cut my life short because of going into such a stressful job again without treating my medical issues. The symptoms have only appeared in the last few months and its caused me so much grief until I found your website. My question is how long is the protocol? Is it… Read more »
The principles are life-long but hopefully some things will improve (less omega-6 in food and a method to permanently control microglia) with time
Hello Dr. Namechek, I think P.O.T.S. is something I’ve been suffering from most of my life. I had fainting spells upon standing as a teenager and young adult. I am one who gets anxiety sitting at a stoplight like you mentioned in your video, and my doctor just smiles when I tell him this. Now that I’m probably perimenopausal and had a spinal leak/headache from an epidural nerve block in my back, I’ve been sick for over a month with rise in temperature and blood pressure. They thought it could be meningitis, so I had a spinal tap where they… Read more »
Sorry, I am not aware of anyone in the region using my protocol.
Hello Dr.Nemechek!
Thanks for taking your time. I am a longterm CFS/ME and POTS patient aged 29 and am still in search for improvement within my illness. Is there already a book for Chronic fatigue/POTS patients you are offering as I have not found any in your shop? (I have only discovered the ones for autism).
Thanks in advance,
K.Neis
Sorry, because of the overwhelming response to the effectiveness of our protocol in children, we are running behind on getting the adult book out.
The kids book will give you plenty of insight on how your condition and how I would approach it.
I understand.. Thank you!!
Ok thank you! I’m wanting to make sure I could get treated by you. But confused, if I can’t take EVOO because of LES muscle how can I take your protocol? I don’t have any signs of SIBO? I’m sorry I live in Ohio so it’s a big decision to make. Are you saying if my POTS is reversed it will fix everything else? Thank you for your time! I really do appreciate it.
All I can say is that there is a manner to move you forward through this.
I understand the concerns about travel, very legitimate.
Once you fix the gut bacteria, much of the food intolerance improves.
I also know medications can cause weakened LES muscle. I do take Immitrex for migraines and have been on amitriptyline for three years and stopped last year. So I don’t know if this is what I have but can this be reversed?
If you have POTS, then it can almost always be reversed.
I started just taking the Olive oil you recommend without the fish oil or inulin for POTS. I thought it was helping my migraines but I started getting a feeling of something stuck in my throat but it’s not. Like I’m having some silent reflux because I do experience alot of belching as well but no heartburn. I read that olive oil can cause your LES muscle to weaken which could cause this. Is this true? I went from having migraines to fibromyalgia than POTS and now this type of reflux. Just seems like everything is going down hill. I… Read more »
EVOO and fish oil can sometimes cause silent reflux especially if SIBO is still present (i.e., no prior treatment with rifaximin).
Can you please explain the role of Low Acetylcholine in autonomic function/dysfunction? Is mestion the miracle some would like to believe?
I don’t find mestinon useful in autonomic recovery. It can alter some symptoms but it does not help in true restoration of autonomic function.
Many times patients who try it are intolerant to it.
Dr. Nemechek,I think I just answered my own question by reading this paper……..http://www.jvr-web.org/images/ICVD-PPPD-Dx-Crit-18Oct16(003).pdf. If I understood correctly it is the autonomic that triggers PPPD.
Yes, you are correct
I think I can speak for the entire community in saying Thank You for your time and attention to this blog. It speaks volumes about your concern for people.
How do you differentiate between n autonomic disorder and Persistent postural-perceptual dizziness? The symptoms seem similar.